Across North Carolina, health systems will again face penalties because too many patients returned to hospitals shortly after being discharged.
In fact, hospitals will pay higher penalties in 2017 than any year in history.
Next year, North Carolina hospitals will see Medicare reimbursements penalized by as much as 3 percent, with rural hospitals generally facing a larger penalty than their urban counterparts. Most hospitals in the state will see a penalty of less than 1 percent. While that might not initially sound like a big hit, consider that North Carolina hospitals take in billions from Medicare, so even small penalties can quickly accumulate to big dollars.
These penalties come as part of a provision in the Affordable Care Act and are intended to encourage hospitals to think about the health of patients as they leave. Historically, one of the drivers of health care costs was patients who had a procedure, but then were re-hospitalized shortly after being discharged.
Now, Medicare is taking a closer look at six common procedures – including heart failure, pneumonia and hip and knee replacements − to see the rates at which patients are readmitted within 30 days of being discharged. The more patients who come back to the hospital – the higher the penalty.
In comparing hospitals across North Carolina, the state has hospitals at all points of the spectrum. Two hospitals face the maximum 3 percent penalty: Northern Hospital of Surry County and Wilkes Regional Medical Center. On the other end, 10 hospitals will face no penalty at all, and another 12 will face a penalty of less than one-tenth of one percent.
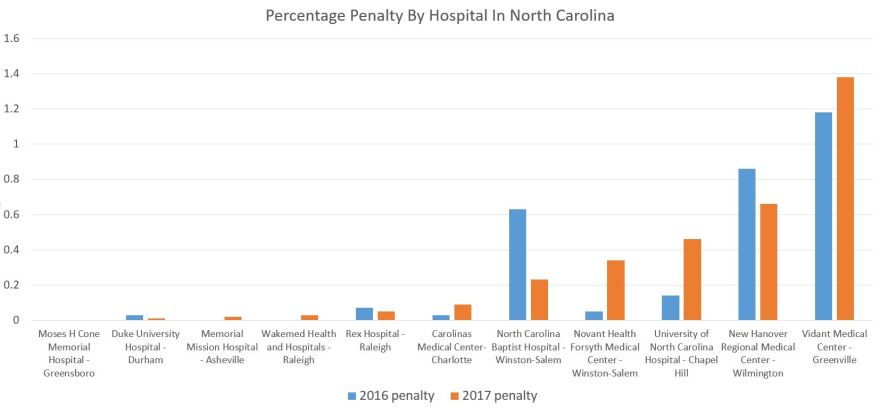
Nationwide, nearly 2,600 hospitals will incur a penalty. While that figure is basically unchanged from last year, the average penalty has gone up, according to an analysis by Kaiser Health News. This trend also played out in North Carolina where the average penalty will be higher next year than for any year in the four years since implementation.
Nationwide, the overall penalties are expected to come to nearly $530 million, a 25 percent increase from last year, according to Medicare.











